by Brady Workman, AuD

Brady Workman, AuD
Many of you may be familiar with the condition of Meniere’s disease or endolymphatic hydrops, which typically consists of episodic rotary vertigo with associated aural pressure, tinnitus, and fluctuating hearing loss in the affected ear. This topic has been covered rather extensively here on the Dizziness Depot; so for those unfamiliar with Meniere’s disease and the proposed theories for the generation of this disease process, click here.
Meniere’s disease can be a rather tricky diagnosis due to disagreement on the exact pathogenesis and the symptom overlap with other diagnoses such as vestibular migraine. Due to this difficulty in making an accurate diagnosis, we as clinicians rely heavily on a thorough case history, and on audiologic and vestibular testing for this diagnosis. Typically after recurrent episodes of Meniere’s disease, an individual will have some degree of vestibular system weakness in the affected ear (most commonly measured = caloric hypofunction) and a low frequency sensorineural hearing loss (low pitch, inner ear hearing loss).
For those interested in more information on the diagnostic criteria for Meniere’s disease, the Barany Society recently released a consensus document, which consists of criteria for definite and probable Meniere’s disease.
Meniere’s Disease and Lermoyez Syndrome
Recently, we saw a patient with a 2 year history consisting of some classic symptoms of Meniere’s disease affecting the right ear; however, rather than the hearing in the affected ear becoming poorer during the episodes of dizziness, this patient reported a subjective improvement in hearing in the affected ear during the episodes.
This patient had been extensively followed prior to referral to our clinic, with documented fluctuating low frequency sensorineural hearing loss in the affected ear in between episodes of dizziness, and with hearing thresholds returning to normal and symmetric during and following an episode of dizziness. This patient had an episode of dizziness 5 days prior to our evaluation and was currently asymptomatic for dizziness symptoms or low frequency hearing loss. At the time of examination, this patient’s hearing test revealed symmetric hearing, with normal hearing thresholds in the low frequencies, but the patient did report some persistent low-level tinnitus in the right ear. Vestibular testing revealed a caloric weakness (reduced response of 35%) affecting the right side. Other testing including rotational chair, video head impulse test (vHIT), cervical and ocular VEMPs were considered to be within normal limits. This patient’s vestibular test results could be consistent with someone with Meniere’s disease; however, the documented fluctuating, low frequency sensorineural hearing loss in the right ear, which improved with the episodes of dizziness, was extremely odd.
Despite these atypical findings, we were not the first clinicians to encounter this constellation of findings, with similar reports first described in 1919 by a French otolaryngologist, Marcel Lermoyez. This is not a common pattern of test findings, as there are few reported cases in the literature. This constellation of test findings have since been coined “Lermoyez Syndrome” with this being regarded as an atypical variant of Meniere’s disease. In fact in Dr. Lermoyez’s original work, he described this syndrome as “Le Vertige Qui Fait Entendre”, which translated to English means “the vertigo that restores hearing”.
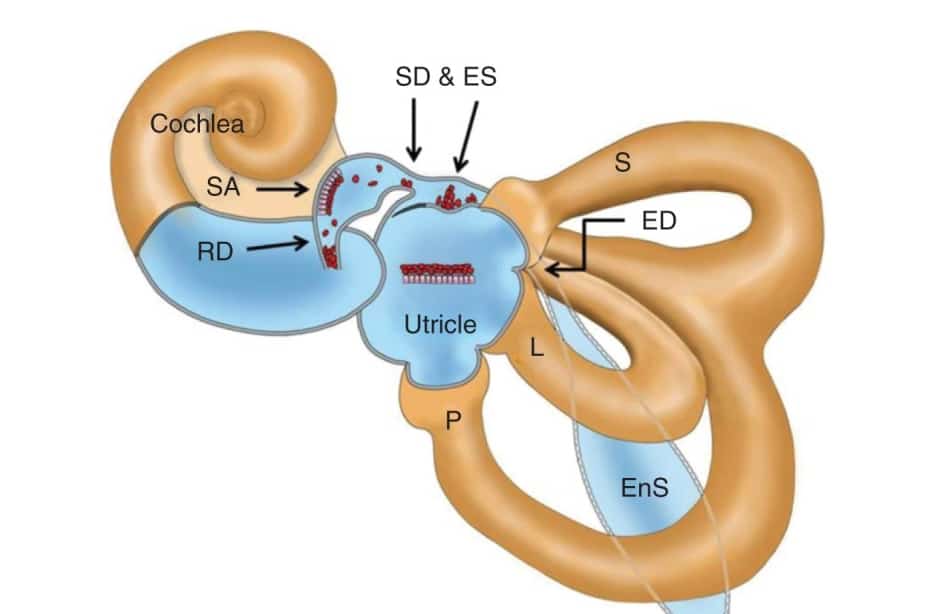
At present, there is much disagreement on this diagnosis, as it seems to be extremely rare with minimal documentation. However, a review of the literature suggests that the cause of these symptoms could be due to a rapid unblocking of the ductus reuniens at the onset of a Lermoyez Syndrome episode. Based off of our patient’s case history, and audiologic and vestibular test findings, it would seem that the most likely diagnosis for this patient would be Lermoyez syndrome.
I do not treat Meniere’s disease or Lermoyez syndrome, but it would seem that if Lermoyez were believed to be a variant of Meniere’s, then the treatments would be similar for both. This patient has previously been managed conservatively with a diuretic (hydrochlorothiazide) and low salt diet, but experienced no symptom relief. Previous intratympanic steroid (dexamethasone) injections provided him with minimal symptom relief. A previous endolymphatic sac decompression surgery relieved the symptoms for only two months. This patient is currently under the care of one of the neurotologists at our clinic and is considering utilizing betahistine for treatment. For those unfamiliar with Menieres disease and the so called “treatment ladder”, click here.
This is not meant to be an exhaustive review for the diagnosis and clinical presentation of Lermoyez Syndrome, but rather to provide some evidence for the existence of this atypical presentation of Meniere’s disease. Many clinicians are unfamiliar with this clinical presentation and may disregard a patient’s report of subjectively better hearing with their episodes of dizziness.
Want more information on vestibular system function in Lermoyez Syndrome? A detailed report can be found here.







A brilliant insight into Meniere’s syndrome provided by Dr. Desmond. In the course of my investigations into hearing changes in my patients with such diseases, I get the impression that the suppression of neurotransmitters in the apical areas of the cochlea may be creating baseline changes , which in turn suppress action potentials triggered relating to environmental sounds. This could be perceived as better perception in the high frequency pick up points and enhance clarity within the speech coding. So, the patient may be reporting less stress in the processing abilities t the apical areas, and translates to better observation of speech inputs.