vHIT equipment is now available from all the leading manufacturers of vestibular testing equipment, and courses are being offered around the country by equipment sales representatives. There is currently no approved billing code for vHIT testing, but that does not diminish the test’s utility.
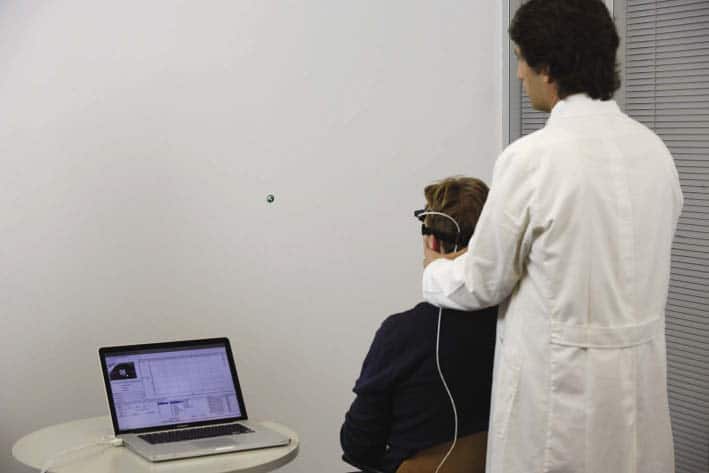
As described last week, the vHIT apparatus records head movement and eye movement simultaneously, which allows the examiner to determine if the high-frequency Vestibular Ocular Reflex (VOR) is working properly. Below I have pasted a photo of the equipment, and a sample trace where the results were normal towards the right, and abnormal towards the left. Just click on the photo to enlarge it.
Random thoughts about vHIT
vHIT has been promoted as an alternative to traditional VOR testing such as rotational chair and videonystagmography. I agree that there is benefit to being able to identify a deficit in the posterior or anterior canals, but vHIT does not provide any information regarding the patient’s level of compensation for any noted deficit. A catch-up saccade and transient visual blurring in response to high acceleration head movement in the direction of a labyrinthine weakness has long been considered a lasting, untreatable legacy of a significant unilateral vestibular injury. So, if you find an abnormality on vHIT, what do you do with that information? Is the patient a candidate for vestibular rehabilitation? How would you objectively measure improvement after rehabilitation?
I don’t know the answers to these questions, but I can tell you that all those questions can be answered based on the results of rotational chair testing (and to a lesser degree, Active Head Rotation testing). I qualify my thoughts based on limited exposure to vHIT, so if there are other opinions, or if I am just plain wrong, please write in and let’s get a different viewpoint out there.
Photos courtesy of Hearing Review.