Hearing Healthcare Market Development Column
With the U.S. continuing to combat the coronavirus, the online hearing test is becoming a crucial vehicle for engaging patients. During a Zoom interview in June, Starkey’s Chief Innovation Officer, Dave Fabry, revealed that during the pandemic’s first wave, patient visits to Starkey’s online hearing test grew significantly.
Starkey’s online hearing test is important because it simulates real-world conditions, demonstrating one of the best practices in Auditory Insight’s new research study, “U.S. Online Hearing Testing and Best Practices for Patient Engagement in Response to Covid-19.”
For the study, Auditory Insight analyzed eight online hearing tests from direct-to-consumer (D2C) hearing aid companies and eight from global hearing aid manufacturers, including Starkey. Auditory Insight defines an online hearing test as an assessment which people take using their own PC or smartphone. Some online tests require headphones, others permit use of device speakers. Online hearing tests, however, are distinct from a full diagnostic exam conducted by a hearing care professional (HCP) in accordance with state regulations.
(Previous HHTM Market Development columns discussed selected results from the study for Listen Lively and Shoebox.)
Simulating Real-World Conditions with Sounds instead of Tones
Regimented, beeping tones are a poor representation for the swirl of sounds, speech, and music that patients hear in their everyday environments. This disconnect inherent in pure tone testing prevents patients from understanding, let alone exploring, the nature of their hearing loss. In contrast, the Starkey online hearing test strives to simulate real-world environments in two ways.
First, the tone test discards traditional beeps for familiar sounds. “When we updated the Starkey.com measure about two years ago,” Fabry said, “we wanted to see if going to more of those everyday, salient sounds,” like birds chirping or coins pinging that patients are likely to experience, would draw them in “to take the test and experience whether they were having challenges.”
Patients who experience recognizable hearing challenges during a hearing test are more likely to acknowledge that they have trouble hearing. This insight is one element of Auditory Insight’s “Patient Engagement Framework for Online Hearing Testing.” The framework focuses on patient engagement best practices rather than clinical best practices or a hearing aid’s underlying technology.
The graphic below shows a screenshot from the sound test when Auditory Insight’s test taker— a male with a moderate, downward sloping hearing loss—completed the assessment in May of this year.
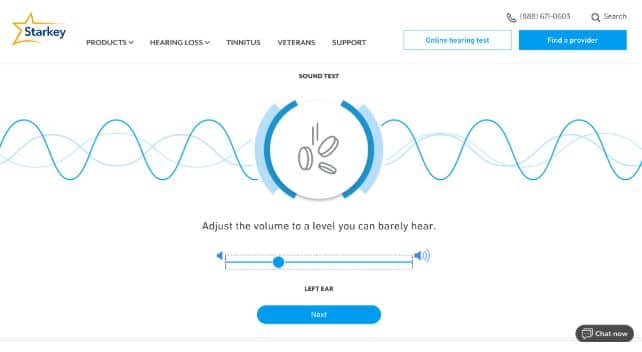
Simulating Real-World Conditions with Speech-in-Noise
The second way that the Starkey test simulates real-world conditions is by pairing the sound test with a words-in-noise test. Presented with four familiar environments, each with a relevant background noise, patients identify a spoken word from four choices.
For example, multitalker babble permeates the restaurant situation, shown in the screenshot below from the Auditory Insight test taker’s same session.
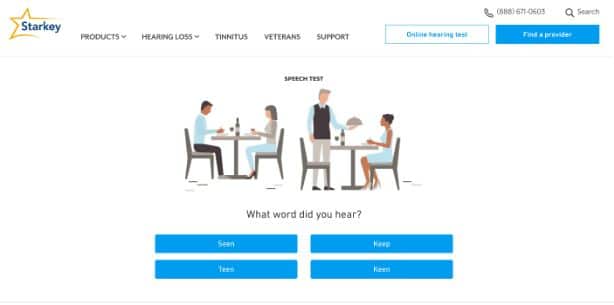
The drawback with speech tests is that their output cannot be used to program hearing aids. By pairing the sound test with the speech test, Starkey is able to gather threshold information while allowing patients to experience their trouble in a familiar way, a patient engagement best practice.
Increase in Online Testing During Pandemic First Wave
“Starkey experienced an approximate 25% increase in organic traffic to our online hearing test since the first wave of coronavirus” starting March 18, Fabry noted in a follow-up email to our discussion.
From Starkey’s perspective, the test is ideal for patients who may not want to immediately see a professional, either because of safety concerns due to Covid-19 or the “combination of healthcare consumerism and aging baby boomers who want to be more engaged,” Fabry added. The online assessment allows these patients to validate the status of their hearing with a convenient measure.
When asked whether Starkey might use the online hearing test in times of extreme social distancing to facilitate a completely digital and remote purchase process for a new patient, Fabry replied, “I would never say never, but that’s not our main focus. We believe very strongly that our technology [is best] in the professional’s hands.” Fabry reported in a follow-up email that “more than 350” HCPs have Starkey’s online hearing test on their website.
Increase in Hearing Care Anywhere Telehealth Platform
In addition to increased website visits to the online hearing screener, Starkey saw a marked increase in HCP usage of its asynchronous telehealth platform, Hearing Care Anywhere. Fabry reported that the growth in the number of sessions on the platform has been “roughly five times what we saw prior to March.”
In the platform’s primary application, at-home adjustments, patients initiate a request through their app. The HCP receives a notification, makes the adjustment, and sends the information back to the cloud. The consumer-patient receives a notification on the app to activate the adjustments.
However, Hearing Care Anywhere currently does not offer in-situ audiometry. Starkey is actively considering adding that capability to its telehealth platform, especially since the company’s Inspire professional platform provided in-situ audiometry for use by HCPs in the clinic prior to the pandemic.
Fabry described the objective of adding in-situ to Hearing Care Anywhere as enabling the HCP, during times of social distancing, to ensure that the patient’s hearing hasn’t changed. “The advantage of doing in-situ Audiometry is you’re using the hearing aid as the audiometer,” Fabry said. “While that doesn’t enable you to calibrate it to a standard, the way you would with a clinical audiometer. . . it is measuring the venting parameters, the microphone location, the depth of the insertion of the receiver in the patient’s ear,” calibrating to that individual patient based on the sounds they hear through their system.
Fabry concluded, “We’re working aggressively on trying to provide as many tools to the professional to stay in contact with their patient as possible.”
**Disclosure: The author discloses that her company consults with hearing device manufacturers and pharmaceutical hearing healthcare companies.
 Nancy M. Williams is President of Auditory Insight, a boutique consultancy advising leaders on transforming hearing healthcare. Nancy partners with senior leaders of pharma and device companies to develop successful commercialization strategies based on deep insight into patient needs, practical understanding of clinical behaviors of audiologists and ENTs, and unique viewpoints on how hearing healthcare is evolving. She holds an MBA from Harvard Business School and a B.A. from Stanford University in Quantitative Economics, both with distinction.
Nancy M. Williams is President of Auditory Insight, a boutique consultancy advising leaders on transforming hearing healthcare. Nancy partners with senior leaders of pharma and device companies to develop successful commercialization strategies based on deep insight into patient needs, practical understanding of clinical behaviors of audiologists and ENTs, and unique viewpoints on how hearing healthcare is evolving. She holds an MBA from Harvard Business School and a B.A. from Stanford University in Quantitative Economics, both with distinction.








Conventional wisdom in audiology assumes that hearing screening must be performed under controlled conditions using a properly calibrated audiometer, and that the relationship between pure-tone and speech recognition testing is weak. In Garrison and Bochner (2018), the authors detail the history and development of a self-administered hearing screening measure, using speech-based naturalistic stimulus materials, that challenges this assumption. Contrary to the viewpoint expressed in the HHTM post that speech tests “cannot be used to program hearing aids”, we establish an empirical connection between frequency-specific hearing thresholds (used to program hearing aids) and performance on an adaptive speech recognition measure administered in either quiet or noise.
Reference: Garrison, W. M. & Bochner, J. H. (2018). Advances in Hearing Healthcare Informatics: The Measurement of Speech Recognition Ability in an Aging Population. New York: Nova Science Publishers.
Thanks very much for sharing this perspective. Dr. Garrison. I’m looking forward to learning more about the speech test you describe. Best, Nancy Williams