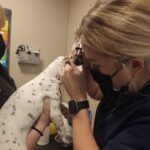
How do you test a dog’s hearing and what exactly is Animal Audiology?
This week, Heather Malyuk is joined by Dr. Kristine Sontrsom Malowski, Director of the Akron FETCHLAB™ at the University of Akron. They discuss all things animal audiology and the fascinating work being done by Dr. Sonstrom Malowski’s at the Akron FETCHLAB™ to evaluate the hearing status in dogs and other animals.
Full Episode Transcript
Heather Malyuk 0:10
Welcome to This Week in Hearing. I’m your guest host Heather Malyuk, and I’m really excited to introduce my guest today, Dr. Kristine Sontrsom Malowski, Dr. Sontrsom Malowski completed her undergraduate and master’s degrees in Animal Science at the University of Connecticut, and went on to earn a dual doctorate in clinical audiology and AuD, as well as philosophy, a PhD from the University of Cincinnati. The focus of her doctoral work was the establishment of baseline normative brainstem auditory evoked responses. There in puppies and special operations multipurpose canines/military working dogs. She is an associate professor at the University of Akron through the Northeast Ohio audiology Consortium. She’s board certified and licensed in clinical audiology, and she holds a certificate in animal audiology from the University of Cincinnati FETCHLAB. On a personal note, I have known Kris for several years now, through research, and for the past year or so she has actually been my superior on a Department of Defense grant, through which we have been studying pharmaceutical intervention for noise induced hearing loss on human subjects. And I will say candidly, that Kris is an absolute joy to work with and for. And even though my role recently ended with our research project, I know Kris, and I will remain very close colleagues for the rest of our careers. And I guess that’s just that’s what happens when you put a couple of passionate audiologists together. So today, though, even though I know her with human work, we’re going to mostly discuss her work with animals rather than humans. So I’ve had the unique opportunity several times to observe and assist at the FETCHLAB at University of Akron. And when I say assist, I mean, I got to hold some puppies. Keep them company for a little bit. And I will say watching her work with dogs has been very eye opening for me, because it’s such a different side of audiology to have a dog as a patient, rather than my patient population, which is adults. And I really respect to this work, which is why I wanted to bring it to this podcast and to the rest of Audiology. So, Chris, thank you so much for taking time out of your crazy busy schedule to speak with me today.
Kristine Sontrsom Malowski 2:24
Absolutely. Thank you so much for having me.
Heather Malyuk 2:26
Yeah, of course I so I want to dive right in. With like a couple of questions to start with. Of course, I want to know your background and how you got started in audiology. But I’m curious, the animal audiology side of things, is that why you became an audiologist because you have a background in animal sciences?
Kristine Sontrsom Malowski 2:45
I would say yes, it stems from a quite an interesting, I would say I come from a non traditional background. Many of us audiologists come from communication sciences and disorders. And because of my background in animal science, I really come from that non traditional aspect. And so when I was in my undergraduate for my Bachelor’s, this was animal science, your basic cows, horses, farm animals. And then my master’s is when I started working with more the bio acoustics which is the sound and the communication of animals. And that includes the anatomy and the physiology and, and all of that intertwined within it. And so I was actually studying for my master’s work, the vocalizations of a beluga whale population in the St. Johns River estuary up in Canada. And we were using Hidden Markov Model, which is like a clustering model to cluster the vocalizations to identify different social groups within the estuary. And so it was interesting because beluga whales are sexually segregated. So you have your adult females and young, in one area of the estuary, you have mixed groups and another area and then you have your like adult males, adult populations in another area. And what we found from that work was that from recording all those vocalizations and analyzing them, the amount of clusters that the vocalizations fell into for the females, and yet, were much greater than those just for your adults. And it’s just saying, because I think of humans and how babies grow up, and they’re cooing, and they’re babbling and making all these sounds, and there’s a lot more variety, if you will, and their vocalizations then when we’re adults, and we have an established communication so that’s really where my interest in in audiology came from. It was my my interest in bio acoustics and the anatomy and the physiology and the communication started of marine mammals, which then during that time we went we also started running their testing or ABR testing in dogs at the University of Connecticut as well. And we were working in collaboration with the CSD department that communication sciences and disorders department and the animal sciences department kind of tag teams and work together to start that testing in those animals and dogs. We also tested marine mammal we’ve also done bear testing and many other species and animals, which I probably won’t focus on much today. But we have done this testing in marine mammals, beluga whales, dolphins, killer whales. And so it’s it’s just a really, really interesting field that I that I love and I’m very passionate about. So I’m excited, I’m
Heather Malyuk 5:16
assuming in Cincinnati, you probably wouldn’t have the opportunity to test marine animals?
Kristine Sontrsom Malowski 5:22
we did. We did a little bit at the Newport Aquarium in Kentucky. We tested some of the shark sting shark Ray, the shark ray that was in the pool we did, which was through bone conduction ABR through the lateral line. And we we did some other, we did ABRs on like, there, they had otters there. So we did a little bit most a lot of the work that we’ve done through FETCHLAB is through aquariums. Not necessarily your your wild populations, I was lucky to have that opportunity during my master’s work to work with a wild population. Yeah, but a lot of the other kind of unique work we do with more of your exotic animals is through the zoos and aquariums.
Heather Malyuk 6:05
So I know your specialty as being dogs, because that’s what I’ve seen you do it did that come about just because that’s where I need was and so it was filled? Or do you have an extra special interest in dogs?
Kristine Sontrsom Malowski 6:18
So we do, we do a lot more with dogs because the test is required by the orthopedic foundation for animals or by some of these organizations for to continue and encourage best breeding practices, especially for breeds that are more prone to congenital hearing loss, for example, like your Dalmatian one in six to one and eight are usually born with some type of with congenital hearing loss in at least one year, if not both. So certain populations, your breeds that have the the white that are white, with or white with some pigmentation or even the blue eyes, those are some of the genetic characteristics that are linked with hearing loss because of the the genetic it’s a it’s like a polygenic trait, if you will. So there’s multiple genes that can contribute to the hearing loss. And so those genes also contribute to what we see with like your white your dogs that have the white and or the blue eyes, for example. Yeah. My interest in dogs I’ve just I’ve loved animal behavior. And I’ve loved working with dogs. I mean, even through animal sciences, I went down the route of am I interested in becoming a veterinarian, and I had a hard time with the sad aspects of that. Yeah. So that’s how I ended up kind of catching on with the audiology and I just didn’t, it kind of stemmed from there.
Heather Malyuk 7:40
I’m kind of curious. You know, I work in a specialty music audiology, and it’s in animal audiology is as rare as music audiology. And, you know, what I find is when I take students or when I was a student, and I knew other people studying it, you know, you graduate and then you kind of end up becoming a typical audiologist. So many do, I’ve probably had close to 60 clinical students, and very few of them are actually working as music audiologists. So with you, somebody like you, you went to school, and you actually made it happen. And to me that’s fascinating. I, I want to know like what the first gig was that you had like, what was so helpful? You graduate, you’re an audiologist and you say, Okay, I’m doing an animal audiology. Yeah. How did you how did you start?
Kristine Sontrsom Malowski 8:26
It was somewhat of like a stipulation of my my job began because when I was doing finishing PhD, or during my entire Ph. D program, I was the manager at UC at the University of Cincinnati’s FETCHLAB, under Dr. Pete Scheifele, who is the founder of FETCHLAB for four years. And so, you know, I said to myself, at that time, when I was doing that, I want to do this when I graduate, and I’m going to continue doing this. And I was getting certified to do it. And I loved you know, I’m just very passionate about it. And so, when I graduated, and I was looking for jobs, one of the I don’t know want to I don’t know that I want to say it was a requirement, but for me, it was somewhat of a stipulation. I wanted to start a fetch lab, and I was looking for an institution that was willing to support that. And that’s kind of how I landed my position here. And we started the clinic. Gosh, it wasn’t, it was less than a year after I started my job here in 2015. We opened our clinic in 2016. And testing dogs ever since. And so there there was a lot of networking and outreach that initially initially just to introduce that we provided our services here and I went to different dog shows and I presented for different like the Dalmatian club, in different locations and things like that. And that’s really how our clinic got started. There was a lot of student there always is a lot of student interest our students are rotated through and they get to run you know, when we have a litter of 12 Puppies, they get to run 12 ABR is and there’s no better experience than being able to routinely you know, one after the other after the other run these ABRs interpret the ABRs have a lot of education and everything that goes on in the clinic, as far as, you know, just teaching generator sites and things like everything they need to know for their clinical doctorate in oncology for humans. Yeah, I
Heather Malyuk 10:11
was gonna say, I’ve seen you teach that. And I learned a lot from watching that. I don’t know that I could ever be the one to place the needle electrode. And I think, you know, that might be tough for review times. But I think you’re absolutely right. It’s such a fascinating way for students to learn electrophysiology. Do you? So of course, a lot of students are interested, do you find that a lot of practicing audiologists is, or any reaching out to you saying, Hey, this is an area I’m interested in? We do
Kristine Sontrsom Malowski 10:38
have, we do obtain those requests every now and then. And we… I think a lot, I think this podcast was great today, because I think what we do is just not known, a lot of people don’t even have we do. And so I do, you know, we do receive those emails, where those inquiries and and it’s really going forward about how to start up a program. And you know, what, what type of occupational setting are you in because it is different between the university setting versus like a private sector, right. So like, at the university setting, we’re regulated by the IACUC, which is the Institutional Animal Care and Use Committee, and they delete everything we do from how many dogs we can see from the consent forms, just really to, you know, ensure that safety for the animals for the and all of the humans, and everybody working in my lab is a member of my current protocol, through the IACUC. So in the private sector, I think the interest is starting to grow. Certainly among those that are getting certified in animal audiology, there’s never, I don’t think there’s enough of a demand to make this a full time position for anyone, but certainly a special like a specialized area, you know, of your job. And in the private sector, really, the challenge is finding the insurance company and making sure you have that liability and everything, because what you’re doing is different, a lot of people don’t understand it. So yeah, you know, be able to, to buy that for
Heather Malyuk 12:01
Yeah, but even thinking of conferences and stuff, you know, I think of how rare again, music audiology is. But you usually see like a music course, at a conference, you know, people are starting to dip their toes in. This is an area where we don’t see anything that I’ve heard Pete speak. But as a featured speaker, talking about testing elephants, or whatever, you know, not like a class on Okay, here’s the one two three of, you know, beginning an animal audiology clinic. And so, you know, when I think of this specialty, I think of it as one of the rarest, sort of most unknown in the field. I so kind of jumping off of that, in terms of thinking about this clinically, or like, what the steps are, I don’t think I’ve ever seen you from start to finish. You know, I’m kind of in and out when I’ve been there. I really would love for you to give me and everyone else listening, an overview of the clinical encounter, actually, from like the first phone call, you get, you know, like, how does how does all of this work? Like what do you ask the breeder or the owner? And then what does the clinical encounter actually look like? And I would love for you to actually really lean into the difficulties, you know, do you sometimes get a dog in person and you say, this is not going to work today? Yes, tell me everything, like from starting
Kristine Sontrsom Malowski 13:19
to go. So clients typically will reach out to me there’s a lot of I did a lot of promoting our clinic opening our doors by going to certain veterinary hospitals around the area. And so a lot of these vets will refer out to our clinic, I either receive a phone call, or I receive an email. And then at that time, I follow up with the owner and I talked to them about you know, what breed Do you have- Is this the litter? How many puppies do you have? We we do a lot of hearing screenings, which I’ll talk about in a minute when I get into what we do. But we also do diagnostic testing, which is a little bit more advanced. And with those dogs, I asked more questions. So you know, your is it an age onset hearing loss, or I’ve been getting a lot of potentially ototoxic hearing loss, or I can’t say it was ototoxic. But dogs that are losing their hearing or going stark deaf, if you will, after being treated with some type of ototoxic medication. Less is known about that in the in the canine world, if you will, compared to our world, but it’s essentially the same, same cause. So for once I talked to the owner and I get them scheduled, they bring their dog or they bring their litter and we bring them into the clinic. We kind of have we have a full sound booth we have the test side and well what we would say where the audiologist sits to do the testing and then where the patient says and so we’re the test side if you will is like our triage room where we’ll bring in the litter we have a pen and we’ll put all the puppies in the pen. This is for litter, of course not a single dog. But at this time we’ll do we’ll talk to the owner we have the owner fill out a consent form that’s regulated by a cook initially and then we go through I usually take a case a case history for The owner, if I don’t on the phone when I speak with them before scheduling, just to kind of gauge a little bit of information, some of my really good breeders will tell you, they have one or two puppies that are either unilaterally or bilaterally deaf, and they know it just from doing testing, and they’ve been breeding for so long. It’s really interesting. So I always I always take a thorough case history from the owners. And then we go through, we do otoscopy on each dog, we apply a lidocaine prilocaine combo, which is like a local anesthetic where the needle electrodes will go, there’s four places on the head. So in front of each ear, top of the head and nape of the neck, we we fill out all of our documentation. So the orthopedic foundation for animals has a specific form for BAER testing or ABR testing in dogs where we fill out the information about the the gender if the dog is chipped or has a microchip, we’ll verify that and we’ll run our reader through that color of the eyes any special markings, which that takes that learning curve in itself, because all different breeds have different markings. And the markings are not the same in one breed as they are in another. So that’s something over the years, I’ve learned more and more about as we’ve had more breeds in. And that’s kind of just like the triage section, if you will, of the day of the testing. Once they’ve all been identified, we’ve had we have their identification, whether it’s a chip number, or name or caller, caller caller identified, then we will bring one in at a time to the other. And that’s where we’ll start the bear testing, and so are the ABR testing. So you’ll hear me saying they’re testing a lot. And just to clarify that the animal community veterinarians, OFA or orthopedic foundation for animals, they all refer to the ABR is the BAER test and dogs, the common language, which is why I’m always saying BAER testing, when I’m referring to ABR testing in dogs. And when I talk about humans, I call it the ABR. That’s good to know. Okay, yeah, so just to clarify that language. But when we bring them in for the BAER test, we have a table and we have several students, you know, several students helping us, we put a thunder shirt on the dog, not so much to serve the purpose of calming the dog, although if it does, that’s great, but more so to keep the wires in place. Because there’s the the wires, the electrodes that go in the head, and then you have the inserts and you want to keep them separate. So
the the thundershirt has a little flap that the electrodes kind of go in, and then we insert those on in the four places of the head. They’re like acupuncture needles, you do need training for that there’s some journal, you lift up the skin, you need training for that, what you would get through the certification if you went through the certification, animal audiology. And then we put this insert in the ear, just like we use the same inserts for dogs that we use for humans, which delivers the sound stimulus and then we run the test. The parameters that we use are a little bit different for dogs, because the OFA, are requires just a basic screening. So not it’s even less complex than a screening that we do for our babies, we really essentially are running a high intensity level. So like 80 dB NHL, or we actually use SPL for dogs relative to sound pressure level instead of NHL because NHL is relative to normal human hearing. And dogs do hear a little bit differently. So we use SPL and there’s a correction factor there but anyhow, so we will start the test we at like a high intensity level. So 80 dB NHL for reference, acquire a recording, we always repeat that recording, and then we move on to the other ear and you interpret that and the the ABR waveform is is similar to how it how it presents in humans, although the latencies are a little bit earlier and the overall overall morphology is a little bit different. So interpretation is a little bit different. I think how clinicians if you will or veterinarians, you know, some some people label wave some people don’t I think what we are doing in our clinics specifically Fache lab is more diagnostic per se more elevated or advanced than what some of these basic BAER com or bear screeners we’ll do that or in other you know that you’re using and things like that. So I definitely tend to go on the heavier diagnostic side also for educational purposes for the students so they really understand what we’re looking at what are the generator sites, where are we labeling What are you know, I teach, I have them on the computer labeling these waveforms and things like that. And we also do masking which is also very much advanced compared to what a lot of these systems are even capable of doing but if we see you know response where it’s questionable we’ll you know, throw some asking if we have a good response in normal hearing ear and then you know, for your
Heather Malyuk 19:53
What about tympanometry? because I know you okay, it was gonna be like I’ve heard you talk about wideband reflectance. and stuff. Yes. Yeah. Curious, like, where does that come into play? Because I’m hearing scoring like screening, which I didn’t realize it’s more of a screening, because what I’ve seen you do is so in depth.
Kristine Sontrsom Malowski 20:10
Yeah, I always do more. Yeah, I mean, even the protocol settings and the number of sweeps Oh, a phase says you have for at least 200 sweeps. For the screening. We typically in humans around 2000. I mean, there’s a lot of differences. It’s a lot, I would say basic for the screenings. Now, for the diagnostic testing, we have experimented with different things. So I, we just published a paper on wideband acoustic events in dogs, which was really exciting because the, that’s a middle ear test. And the system that we have does not require you to maintain that seal. And that’s the challenge with the dog. So dogs have both a vertical and a horizontal component to their ear canal, which makes any type of you know, obtaining a seal or anything like that challenging because of just the anatomy of the outer ear. And so we recently experimented with wideband acoustic and mittens because the system we have is a soft insert that goes in the ear, and it doesn’t require that seal or that pressure because that also can upset or startle the dog there and publications out there on tympanometry. And dogs. Not much. The literature is is not flourishing, if you will, there’s a it’s a it’s an open area for anyone interested, but certainly they have done tympanometry. And the results look similar the the similar to what we see in humans, the wideband acoustic admittance that we did, the patterns were very, they were a little bit different in terms of the peaks and how they in the troughs and how they fell. But they were similar, but different, if you will, there’s a publication on that for anybody interested that was recently published in JASA as is really, because that’s the first time that’s ever been published to our knowledge or that works been done. And then also, for a diagnostic, we will also run otoacoustic emissions if the dog is compliant. There are some vets that will sedate dogs or require sedation, we certainly don’t require that for the clinic. I’ve tested hundreds and hundreds, if not 1000s of dogs since I started doing this. And you know, rarely does a dog need to be sedated unless you’re dealing with like a military working dog, a police dog or a dog that is you know, where you’re at where you could get injured,
Heather Malyuk 22:19
is that even in the scope of practice,
Kristine Sontrsom Malowski 22:21
not for audiologists, okay, so if you need a dog to be sedated, that has to be done by the owners, by the dog’s veterinarian, okay, administered by the owner, we don’t do anything with that. However, we have specific paperwork that needs to be completed by the owners veterinarian if the dog is sedated, and and I mean, I’ve only had I don’t even know that I’ve ever had a sedated dog since I’ve been doing this clinic. Now that I’m thinking about it, but definitely out of our scope of practice. So
Heather Malyuk 22:52
well, I know you’ve done work to with canine handlers, like you mentioned Military Police stuff, because one of them, you have a publication on that correct? Yes. Take her poster or something.
Kristine Sontrsom Malowski 23:03
Yeah, we did. We we did. I had a public noise, or what were we k9 handlers It was the it was the handler.
Heather Malyuk 23:12
And it was just the owners. You didn’t look at the dogs as well. Right? You were just looking at noise induced hearing loss in the handlers
Kristine Sontrsom Malowski 23:17
Yes. And we canine handlers to non canine handlers and looking to see if the hearing losses that we found in the handlers vary between the two groups. And so but we didn’t do any testing in the dogs, I have these dog in a year or two ago when I was working on that on that specific research. And there was no way I was going to test that dog. It was too they’re way too high, strong. They’re just you really they really need to be put under sedated in order to do that type of test.
Heather Malyuk 23:46
I would say that’s what I was curious about, like who who shows up and you say, Okay, we’re not doing this. Yeah. Well, the specific dog
Kristine Sontrsom Malowski 23:53
we hadn’t started, like ripping the foam out in between the sound booth. It was it was a little. And it was just they’re just too high strung. I mean, naturally for what they need to do. They’re working dogs. They’re very Yeah. And so I just said, we’re not going to go there. We could have, you know, the owner could have gotten the dog to sit for the test. But the problem is we’re running electrophysiology, so you have a dog that’s moving around a lot or panting a lot or is not willing to sit somewhat still for the test. It presents a challenge.
Heather Malyuk 24:22
Yeah. But like, where do you draw the line on aggression? Because obviously, if a dogs coming in and they’ve never met you before, and they get a little nippy or something, you know, we have certain lines we draw with patients, right? Where we’re like, okay, if you’re gonna act that way, I can’t see you. Well, what where’s the line for a dog?
Kristine Sontrsom Malowski 24:40
Usually, it’s the dogs that are shy or timid, that are more of a concern than even you know, I don’t typically have a dog that walks in the door. That’s just an aggressive dogs because we typically just don’t see them but I’ve had dogs come in that are very, very shy and timid and, you know, maybe their tails between their legs or you know, they’re maybe they’re on And like shaking, you could just tell that they’re more timid. Those are the dogs I’ve been bitten by those are the dogs that if they’re not comfortable enough, and I can’t even look in their ears or apply lidocaine or anything like that, I tell them that they’re going to need to get a sedation from their vet if they liked it. The tests are usually what I do with the dogs that need to be sedated or put under us, I’ll refer them to some of the vets that we collaborate with that do this testing. Okay, at university. And so usually I’ll refer in that case, if a dog needs to be put under if if we’re at risk, because I certainly am not going to put you know, my students or myself in any in harm’s way in that regard.
Heather Malyuk 25:34
Yeah. Would you ever have the owner hold the dog? Or is that typically..? Yeah,
Kristine Sontrsom Malowski 25:39
yeah, it just depends on the dog. We’ve, you know, if the dog is more comfortable being held by the owner, I let the owner Hold on. And, you know, and otherwise, sometimes they’re not sometimes the dog the dog responds better when the owners not even in the room, and usually the owner gauges that, and Can you guide me on that? Um, but yeah, so and I think, what was it? Oh, no, that was that. So I was just thinking back to the diagnostic testing, because that’s, we typically will just do the otoacoustic emmisions, that’s what I was gonna say the BAER test for diagnostic is a little bit different to us, because we actually estimate thresholds. So that’s the difference in difference between the BAER test for a screening where we just test, you know, one run one run repeated at a high intensity level, and then we also will test for diagnostics will estimate thresholds, so we’ll drop until we lose our response. Okay. That was it for like the, versus the screening. As far as the process goes, and then really, after that we on hook the dog, there’s a lot of love and positive reinforcement. I mean, we want to keep it a positive experience for the dog, especially your puppies that will remember these, you know, moments potentially, or life, so we really want to keep it a positive experience. There, we will give treats if needed at the end. We also at that time, will counsel and educate the owners depending on what we find. So thing is normal, we’ll fill out the paperwork, they submit that we’re good to go. If there’s hearing loss, if it’s like a diagnostic and there’s some level of hearing loss, I just usually counsel and educate kind of using the criteria that we do for humans right now. This is something there is no real universally accepted norm, if you will, for normal hearing for dogs. And that’s something I’ve been working on for many years in terms of collecting data to try to create, you know, your like your degrees of hearing loss for dogs. Similar to what we have for humans. All I can do now is counsel based on what we have with humans and and then educate the owners in terms of whether it’s a deaf dog or unilaterally deaf, unilaterally deaf, usually localization is the biggest issue. They’ll make great pets, we don’t encourage doing. If you’re really deaf, bilateral deafness, that’s when you want to start training using like methods of American Sign Language hand signals, getting the dog to look at you is number one, socialization is so important. I’ve seen
Heather Malyuk 27:59
that there, which was my first experience seeing someone use sign language with the dog, and our our mutual student. And you know, and she brought her dog in and she would I think it was my first week doing research with you. And her dog was in and she kept I can’t remember the signs. But she kept saying good girl to the dog. And every time the dog would see those signs, the tail would wag. And I was like, this is just the cutest, most amazing thing I’ve ever seen that that dog has communication, you know, that they can learn to work with whatever they’re given, and they want to communicate and that you were, you know, helping that process. I thought that was so amazing. And the other thing I wanted to ask just a more basic question. How many are you seeing? I feel like when I was there, of course, I was around for about a year or so a couple days a week, and I feel like you were always running to see a litter of 10 puppies or, or there’s like an adult coming in and like, oh, gosh, 15 Dalmatians just showed up. But like, how many a week are you typically testing.
Kristine Sontrsom Malowski 29:00
So we test one day a week typically, in the morning and or afternoon if needed. And so it just depends There’s certain times of the year that we’re busier spring, because a lot of breeders like to breed and so the pups are born when it’s nicer weather out. see quite a few also in the winter, around Christmas around the holidays. Christmas puppies, I would say as far as we typically will have one like usually once a week we’ll have a litter in or I might have a couple of appointments where I have a few dogs or a single dog and then a letter. It just varies it really I think we slow down a little bit after after COVID and we’re starting to pick up I mean, I’m booking out into October right now
Heather Malyuk 29:46
when people are driving like a couple hours to see ya, you know, that was something that shocked me as well as I mean obviously there aren’t providers like you and people were calling you from other states and then driving in to see you that day. doesn’t need me as well, because again, we deal with that music audiology, you know, and I was like, and this is what this is what specialties are in audiology, someone will find you and they’ll come see you. And just so you are specialized in a lot of ways. And just to take a couple minutes. Well, you’re unique audiologist, I love alternative audiologists it because there’s so much more to our field than what than what we typically see. And I wanted you to just touch on some of the other hats you wear. I know you through hearing conservation, you know, and that’s a hat you wear. But you’re also, you know, talk about just for a couple minutes, the courses you teach, you know, and how broad your knowledge base actually is.
Kristine Sontrsom Malowski 30:40
So I teach the vestibular courses here are the introductory, introductory to, I think it’s balance assessment and management. But anyhow, the introductory vestibular course is also the advanced vestibular and the advanced electrophys course and the labs that are associated with those courses. I also have taught the seminar in audiology, which is a research based course. I’ve also I’m also teaching multicultural, multicultural issues for the audiologist for our first years. And then an array of just the clinical courses that we have here, which like the students are rotated through fetch lab through one of their clinical courses. And I really have an interest like you have there. This is why we connect so well, I really have an interest in unique populations. So my work with the police officers that I’ve done, it is inspiring for me, and it really is an underserved population, the amount of noise induced hearing loss I found in that across that population is it we just need to keep raising awareness and promoting better care for these populations. Yeah, I’m also I’ve done quite a few interprofessional activities here at the University. I work with a team here through a veteran grant that we have to for our own students that are either veterans or still active in the reserves that have sustained traumatic brain injuries or have cognitive deficits that need care. And we have an interprofessional team between speech language pathology, audiology School of Social Work, counseling, maybe there’s an interprofessional team here, where we we run all the way from your basic your hearing testing to your tests of auditory processing all the way through with speech therapists do it’s a it’s a CT CCT program, cognitive compensatory training program. And that has been valuable for some of our students that have had those types of disorders or issues. If you have also done here, I manage as part of one of the clinical courses, the hearing screening program that we have here, where we send our students out to our local schools, for screenings from all the way from, you know, we’ve done some daycare, but usually from the elementary level up through your high school level, we work with our local school districts. I don’t know what else do I do?
Heather Malyuk 32:57
It’s just a lot. You know, when I’m really busy people I know you’re always at the top of the list. And I know you’re a tough teacher too, because I’ve watched you grading things. Sometimes your tests are hard, and you’re very tough. And I think you know that the hearing conservation side of stuff i i Of course find fascinating night. And I didn’t mention that you and I were going on site to shooting ranges with students and testing hearing after shooting looking for shifts. Fascinating. And again, that’s another specialty another huge area of Audiology. This is a totally underserved population and talking to those guys and saying like, Do you realize what you’re exposed to, and they really just don’t have the educational component? Yes.
Kristine Sontrsom Malowski 33:41
I have to mention this, because I think we talked about this when you were here. But last week, we tested our entire rifle team here at the university. It was a full day event, we tested 15 students that are part of our rifle team. And the and all the coaches have been tested with support of our athletics department. In and we also, we also held a hearing conservation education session that afternoon and it was just a really, really successful event. And it’s awesome in that we laid the groundwork for so that we can continue annually testing these students that are exposed to firearm noise as a as an athlete as athletes, and that will be over the next several years and that are that have been shooting since they were eight years old or and so that was a really, really, really good event that we started here and we’ll monitor these guys for you know, their duration while at the university, which Yeah, and
Heather Malyuk 34:32
you’re setting up good habits for life. You know, that’s the thing is reaching out to those populations. They’re not in school getting, you know, while they’re in school at Akron, but I’m talking about they’re not in middle school, having a hearing screening, whatever you’re teaching them the value of an annual hearing test. And that’s I really think all audiologists should be doing that is reaching out to these younger populations and saying, Hey, let’s look at your hearing and make sure it’s stable every year. You know, and the value in that and I know we kind of get off the animal audio but she’s Just because I can’t help but lean toward hearing conservation. Do you ever do hearing conservation with dogs? I learned the other day about ear plugs for horses? Yes. And so is that a thing for dogs?
Kristine Sontrsom Malowski 35:12
Well, I was just gonna Yes, I was just gonna mention hearing protection devices, because that’s part of the education that we offer to these students on what some of them are doing. I won’t repeat on here, but it’s certainly not hearing protection device. But for dogs, I mean, usually the kind of the conversation about hearing preservation, if you will, comes up for dogs that are exposed to noise like your police dogs, or military dogs. Or the other conversation is if there’s a dog that is undergoing like a long term antibiotic treatment, that are potentially exposed to the ototoxic medications. And so more for the hearing conservation and the noise induced hearing loss, they do. Actually, Dr. P Shively out of out of Cincinnati, one of my if not my ultimate, best mentor. But he developed in collaboration, I believe, for their engineering department. And for the DOD, or the Department of Defense, I believe. They’re called caps. And they’re actually hearing protection devices for dogs that go over the ears. So their mom are designed to be not to be cumbersome, if you will, because sometimes these dogs will also wear goggles and things on their eyes as well. And they were also designed so that you the handler through the hearing protection device can communicate with the dog. Because these dogs that this is really where the my PhD research stemmed from is that military working dogs were being flown, like in helicopters with their handlers, and then they were being dropped, you know, and then they weren’t responding to their handlers at all, because the dogs never had hearing protection. And the handlers did everyone else in the helicopter did right. And some others were saying, you know, my my dogs not responding at a critical moment when they really need to be responding. And there’s that loss of situational awareness. So that’s what really sparked a lot of that research and the development of these hearing protection devices that they do currently have for
Heather Malyuk 37:04
Yeah, so that is awesome. Then I you know, and again, talking about an underserved population, dogs who are exposed that nobody’s thinking about, I mean, that’s just fascinating to me, I can’t believe we’re already almost out of time, because I have a million more questions I want to ask, but, you know, if there are audiologists listening, or students listening, and they’re curious about expanding their services in this area, or even just expanding their knowledge, you know, if they want to read more, where would they start? Like, do you have any recommendations for certain books or websites or anything? I would say,
Kristine Sontrsom Malowski 37:39
um, so fetch lab. It’s a big acronym. It stands for the facility for the education and testing of canine hearing and the laboratory for animal bioacoustics. I won’t quiz you on that at the end. However, it was developed by Dr. P. Shively. He’s the founder. And that program is now at the University of Cincinnati. We have it here at the University of Akron, and also at the University of Northern Colorado, I believe, have a base like in Alaska and are developing another one in the South West somewhere. Anyhow, it’s expanding, and it’s growing. And what I would say is the certification and animal audiology that you can obtain through that program is extremely valuable for any audiologist that’s interested in doing this. Because like I said, earlier, we come maybe not myself, I’m non traditional, but most audiologists come from a CSD background, and they don’t have the background in animal behavior. And animal behavior is critical to just like we were talking about when do you say, you know, we’re not going to do the tests on a dog, you really have to understand, you know, their behavior, their signs. Also understanding how they hear their anatomy and physiology, the ear, which is a little bit different than humans, not greatly, but a little bit different, their frequency range of hearing is a little bit different. And within that certification, you also learn about other animals, including, you know, marine mammals, birds have exotics, as well as animals. And so there’s a lot of specialized individuals that will also speak as part of the certification. Dr. Pete’s wife is a Exotic Animal Trainer, she went to school for that. And so, you know, I would encourage anybody that’s interested to look into that program. Currently, you can obtain the certificate through the University of Cincinnati in northern Colorado, you can obtain your hours here, but we don’t currently have the certificate program here at Akron. But because of my collaboration with Dr. P in Cincinnati, the courses are all online. So you take the courses online, you just have to fulfill your hours at one of our clinical locations for the practical requirements. So that’s what I would recommend because that will really help with the education piece. It is a 12 credit certificate program. Also, you know, just I guess, I’m thinking of like, if you wanted to start a program like this on your own, it’s important to consider, you know, how are you going to be regulated and liability those are important, you know, and we collaborate with the veterinary community as much as we can we have an inter, you know, disciplinary or interprofessional relationship with a veterinary community with animal behaviorists. And that’s what makes this work and that paper you know, I was telling you why being acoustic admittance paper we collaborated with Dr. Lynette Cole down at Ohio State University and she’s a great colleague of mine and I refer patients to her you know, often if I feel like a dog will need to be put under sedated or or even middle ear issues because that’s she specializes in dermatology and middle ear issues and so just you know, keeping networking talking to people in educating yourself looking at you know, the requirements and making sure that you’re protected and you’re you’re working with the right group of people is important, but it’s an awesome field. If I can say anything, I love what I do. I’m very passionate about it. I’ve been doing this for many years now I will probably never stop no matter where the road you know, where I ended up. But you know, there’s there’s so much that we can still learn in this field. I think we like music audiology, there’s just like so much we can do and, and learn and, and, and educate. And so I really am passionate about it. Really excited to be talking to you about it today.
Heather Malyuk 41:20
I just love that and it’s your passion definitely shines through for sure. Even on a video call like this, not just in the clinic, and I really appreciate you taking time to talk about it. I think. I’m sure there are many people listening who have never heard of this area of audiology before and it truly is fascinating. And thank you again so much for your time. Absolutely.
Kristine Sontrsom Malowski 41:42
Thank you so much for having me how there was a pleasure. Thanks
Be sure to subscribe to the TWIH YouTube channel for the latest episodes each week and follow This Week in Hearing on LinkedIn and Twitter.
Prefer to listen on the go? Tune into the TWIH Podcast on your favorite podcast streaming service, including Apple, Spotify, Google and more.
Image gallery below from the Akron FETCHLAB™ (click to enlarge)
About the Panel
 Heather Malyuk, AuD is a musician and audiologist who hails from Northeast Ohio but is known internationally as an expert clinician and public speaker in the field of music audiology. Dr. Malyuk owns and directs Soundcheck Audiology and is also a researcher at the University of Akron, on a team studying pharmaceutical intervention for Noise-Induced Hearing Loss. As Tuned’s Head of Audiology, she feels blessed to be able to use her unique audiologic background to help audiologists connect with a modern patient base.
Heather Malyuk, AuD is a musician and audiologist who hails from Northeast Ohio but is known internationally as an expert clinician and public speaker in the field of music audiology. Dr. Malyuk owns and directs Soundcheck Audiology and is also a researcher at the University of Akron, on a team studying pharmaceutical intervention for Noise-Induced Hearing Loss. As Tuned’s Head of Audiology, she feels blessed to be able to use her unique audiologic background to help audiologists connect with a modern patient base.

Dr. Kristine Sonstrom Malowski is an Associate Professor of Audiology at the University of Akron, Northeastern Ohio AuD Consortium and the Director of FETCHLAB™ Akron. She holds a Bachelor’s and Master’s degree in Animal Science from the University of Connecticut and a dual doctorate in Clinical Audiology (AuD) and Hearing Science (PhD) from the University of Cincinnati. Her research interests include auditory electrophysiology, neuroaudiology, noise-induced hearing loss, hearing conservation, animal audiology and bioacoustics. Kristine is a licensed, board-certified Audiologist, a Fellow of the American Academy of Audiology, holds a Certificate of Clinical Competency in Audiology from ASHA and a certificate in Animal Audiology from the University of Cincinnati FETCHLAB™.