This is Part II of a post by my doctoral student, Brady Workman, B.S. Last time he described what VEMP’s are actually measuring. This week, he focuses on clinical applications, basically, “What are they good for?”
(VEMP) Vestibular Evoked Myogenic Potentials: Now what do we do with them?
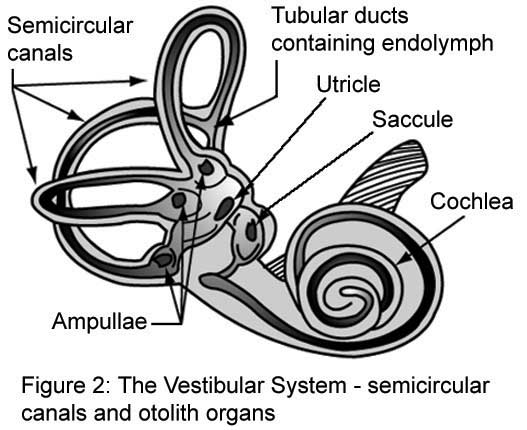
In the last post, we briefly talked about what VEMPs are and where they originate. This week’s post will focus on how VEMPs are utilized clinically, as well as potential future uses for VEMPs. Just to recap the previous post, cVEMP (c for cervical) is primarily a measure of saccule “up and down sensor” and inferior branch of the vestibular nerve function. The oVEMP (o for ocular) is primarily a measure of utricle “side to side/front and back sensor” and superior branch of the vestibular nerve function.
Currently VEMPs are most commonly utilized for independent assessment of the otolith organs (saccule & utricle), investigation of the inferior branch of the vestibular nerve in the case of cVEMP, and to identify potential superior canal dehiscence. Traditional means of vestibular assessment only measure the function of one of the five primary organs of the vestibular system (horizontal semicircular canal) and the superior branch of the vestibular nerve. Independent assessment of all vestibular organs and both the inferior and superior branch of the vestibular nerve seems essential to best understand and determine outcomes for a patient with a vestibular system injury.
A superior canal dehiscence is a “thinning” or opening of the superior canal of the vestibular system, causing dizziness symptoms associated with sound or pressure changes. Click here for more information on superior canal dehiscence. Those with superior canal dehiscence tend to have abnormally low VEMP thresholds as well as large amplitude measures in the affected ear. Click here for more on VEMP interpretation in superior canal dehiscence.
VEMPs may also be used in conjunction with other measures to assist in the diagnosis of Meniere’s disease, vestibular schwannoma/acoustic neuroma, and other central vestibular disorders, to name just a few.
VEMPs have been implicated as useful in differentiating Meniere’s disease from other vestibulopathies. Individuals with Meniere’s disease have an over-accumulation of endolymph (one of the inner ear fluids), which may cause damage to the utricle and/or saccule. The incurred damage is then likely to cause a lower amplitude VEMP response in the affected ear. Click here for more information on VEMPs and Meniere’s disease.
A vestibular schwannoma or acoustic neuroma is a benign tumor that typically grows on the hearing or balance nerve, which can reduce vestibular input to the brain, as well as affect other nearby nerves and neural structures. Click here for more information on vestibular schwannoma/acoustic neuroma. One would expect VEMP responses in the presence of vestibular schwannoma/acoustic neuroma to be reduced in amplitude or absent on the affected side due to compression of the nerve from the tumor. Click here for more on the VEMP profile of someone with vestibular schwannoma/acoustic neuroma.
A central vestibular disorder could refer to any disorder or abnormality along the brain or brainstem pathways. Due to the different neural pathways of the oVEMP and cVEMP, valuable localizing information can be provided through their implementation. VEMP abnormalities have been shown in patients with multiple sclerosis, basilar migraine and lower brainstem stroke. Click here for more information on VEMPs in central vestibular disorders.
Currently VEMPs are useful, complimentary measures that may be utilized with other means of vestibular assessment in order to develop a more comprehensive understanding of each patient’s vestibular system. Because VEMP measures are a more recent discovery than other more traditional means of vestibular assessment, the relative uses for them are narrow and not as well understood. However, it seems that in the future, new uses for VEMPs will be identified and it is likely that their clinical implementation will grow as well.