Use of ear tubes – also known as tympanostomy tubes – has been a common solution to chronic ear problems in children for many years. In fact, myringotomy with tube insertion is the most commonly performed outpatient surgery on children in the US. More than 700,000 children undergo the procedure annually.
The purpose of tympanostomy tubes is to aerate the middle ear and relieve excessive fluid build-up. Unfortunately, a significant number of those tubes fail, which can lead to painful complications, which may require invasive treatments and potentially lead to the need for additional surgeries.
The idea of improving tympanostomy tube technology started when Harvard School of Engineearing and Applied Science (SEAS) graduate student Nicole Black took a clinical otolaryngology class at Massachusetts Eye and Ear. Classmates in the course had looked inside her ear and noted the presence of scar tissue that was due to ear tube placement as a child.
“I started thinking, the scar tissue on my eardrum is probably not helping sound conduction. There has to be a better way to treat chronic ear infections. That was the starting point for me to think of this project in a different way, in that this is actually something that could potentially improve the lives of millions of patients.” –Nicole Black
Black then collaborated with Ida Pavlichenko, a postdoctoral fellow in the lab of another SEAS researcher. The pair soon met with ENT surgeons Aaron Remenschneider, an investigator at Eaton Peabody Laboratories, and Elliott Kozin, Chief Resident in the Department of Otolaryngology at Harvard Medical School, to discuss how novel technology could potentially improve patient outcomes.
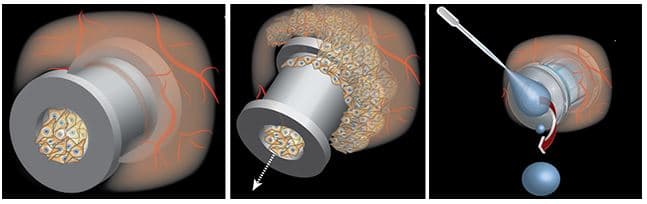
Tympanostomy tubes become clogged (left) or may extrude too quickly (middle). Current designs also offer limited ability to treat ear infections topically (right.) Image courtesy of PionEar, via Harvard University.
“As soon as Nicole and Ida discussed their research on slippery surfaces, one obvious application arose. As surgeons, we spend a lot of time putting in ear tubes, but many limitations with the technology remain. Tympanostomy tubes in children often become clogged with cellular debris, which requires them to be replaced through a revision surgery under anesthesia. In addition, tubes may extrude too quickly or remain in the ear drum for an extended period of time, also requiring an additional procedure.”
–Aaron Remenschneider, MD
PionEar: Re-thinking the Ear Tube

PionEar team members: Aaron Remenschneider, Nicole Black, Ida Pavlichenko, and Elliott Kozin. Image courtesy of PionEar, via Harvard University.
Due to their size, current tubes present significant challenges to effectively treat infections using topical ear drops. PionEar’s goal is to create ear tubes that won’t clog as easily and can improve drug delivery to the middle ear.
Using anti-fouling technology from the Aizenberg lab, and novel materials from the Lewis lab, the PionEar team aims to develop an “easy-to-manufacture, liquid-infused ear tube that prevents cells from sticking to the surface”. According to Black, prototypes they’ve created are smaller and easier to implant than current models.
The team’s innovative approach recently led PionEar to win a $75,000 Harvard President’s Innovation Challenge Contest. Other funding, including grants from Mass Eye and Ear, will help them further develop and commercialize the new tube designs.
The team is said to be considering plans to formally launch PionEar as a new company soon, and may explore venture capital investments in the future.
In comments to Boston Inno, Pavlichenko said she sees additional opportunities following the development of the ear tubes, “we ideally would like to open up doors to other problems of middle and inner ear, such as hearing loss”.
Source: Harvard, PionEar







