In Part III of “Trimming the Sails” by Dr. Christopher Schweitzer continues his provocative treatise as to why hearing aid market penetration fails to meet desired goals. This builds upon many of the posts that have been provided previously on this HHTM site, including a ten-part series on hearing aid dispensing. Dr. Schweitzer is Director of HEAR 4-U International; Chief of Auditory Sciences at Able Planet, Inc.; and Senior Audiologist, Family Hearing Centers in Colorado. As with all content written by guest authors, the opinions expressed are those of the author, and do not necessarily reflect those of HHTM (Hearing Health and Technology Matters).
Wayne Staab, Section Editor
The Rise of the Oligopoly
To a studious consumer searching for clarity in the blurry seascape of hearing aid company messages, boastful product innovation announcements, private and corporate dispensing offices communications, mail order and online options, one fundamental fact may rise from their “due diligence” investigation. Up to 90% of the hearing aid market is traceable to a group of six manufacturers.
That same investigator may discover a highly concentrated supply chain of essential components such as microphones, speakers, and circuits. Additionally, there is considerable sharing and pooling of resources for signal processing software and interface solutions. This naturally leads to questions about prices and influence. In classic vertical integration and consolidation maneuvers, the major manufacturers have jockeyed across the distribution field, vigorously buying or opening dispensing chains (or brands) over the past ten or more years. An oligopoly is a situation in which a few firms dominate a particular market, often the outcome of a process of consolidation. “An oligopolistic industry is dominated by a small number of large firms, each of which is relatively large compared to the overall size of the market. This generates substantial market control, the extent of market control depending on the number and size of the firms”1.
Examples of oligopolies can be found in airlines, medical insurance, beer and soda products, cell phone carriers, gasoline, book and music publishing, and cable providers, to name a few. In the 1970s, approximately 100 companies were listed as hearing aid manufacturers from which the author could choose for a client. Prominent brand names such as Radioear, Zenith, Sonotone, Telex, Vicon, 3M, and Maico (among many others) have largely disappeared from the menu of product choices. Many others have been systematically absorbed or eliminated by the dominant six, which continue to maintain a scattering of secondary brands as branches owned or controlled by a holding company or directly by the brand at the top. A few smaller independent hearing aid manufacturers do remain and new upstart entries periodically appear in the shifting supplier seascape. Many of the second- and third-tier companies are essentially branded assemblers of core components, namely digital amplifiers, transducers, and licensees of software platforms.
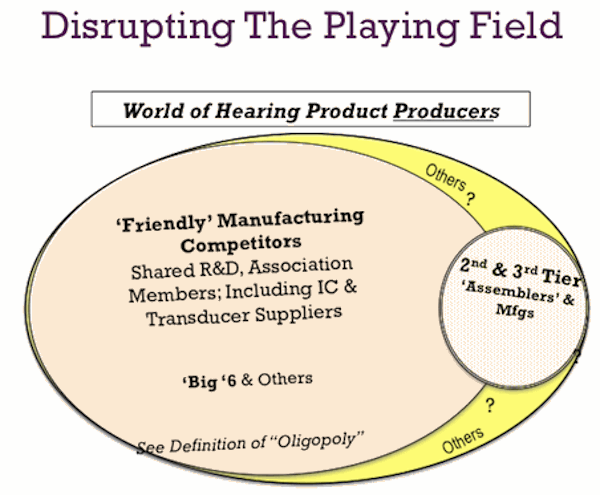
Figure 3. Conceptual illustration of the Product Producer Landscape dominated by a (now) relatively small group of manufacturers.
Hence, one of the consequences of the vigorous consolidation in the hearing aid industry in recent years has been the appearance of a cartel-like cooperation among a relatively small number of “friendly competitors.” Figure 3 attempts to illustrate the situation as of 2013. One way for the dominant oligopoly of top tier manufacturers to constrain competition from new and potentially disruptive entries is to push the regulatory agencies, such as the FDA and/or the Federal Trade Commission (FTC), to rein in new entries that offer disruptive pricing, technology, or distribution. This tactic is somewhat ironic in that those same regulatory agencies, which are often viewed as impediments to profit and market expansion, become the “go to” strategy when unwelcome competition arrives at the dance. Letters to the FDA have been historically launched from the hearing industry trade association as a means of securing barriers to entry and to “protect” consumers.
Product Delivery: The Consumer Interface
Having touched on the supply chain, the next area of relevance in the hearing products seascape is the routing of the devices to the consumer, that is, the distribution channel. Delivery options include medically oriented ENT and audiological offices, retail chains with hearing centers, manufacturer-owned or franchised hearing centers, mail order, the Internet, and Veterans Administration hospital clinics for those who qualify for VA care. Here again blurriness and changing winds are encountered. Figure 4 attempts to draw out some of the non-crisp boundaries of the distribution modalities. Dispensing practices, independent and corporate-owned, are naturally the most traceable component since their numbers are largely under the purview of the manufacturers and their member organization, the Hearing Industries Association (HIA).
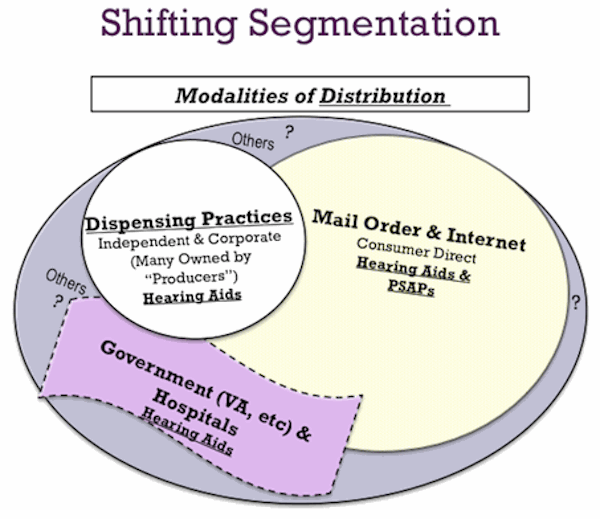
Figure 4. Conceptual illustration of the Distribution Dynamics that inter-play for the consumer shopping for a hearing help product.
Until recently, PSAPs have generally not been available through dispensing locations. They have instead reached consumers almost entirely through online or mail-order sources, despite systematic professional and industry-organized opposition. Increasingly, however, these products may be found among the health related options of pharmacies and big box retailers. But a sea of change in these practices appears to be stirring. Given the decreasing trajectory of Average Selling Price (ASP) in the past two years2, post-recessionary declines in consumer discretionary income, and more austere benefit packages from third-party payers and government-funded programs, dispensers must look for ways to maintain revenue levels.
To be sure, mail order, online hearing aid sales, and non-medical PSAPs from any source have been reflexively demonized by audiologists and dispensers (with encouragement from major hearing aid companies). PSAPs are factually “assistive listening” products which, by virtue of advances in technology and production, have considerable similarity in form and function to higher priced hearing aids. Brisk sales and low returns for companies like Able Planet (with which the author is affiliated) that pay attention to sound quality and robust product choices demonstrate a market size and readiness consistent with the Figure 1 model’s assumptions in Part I of this Series. Perhaps PSAPs have the potential to help dispensers negotiate the turbulent sea winds. Can this disruption deliver opportunities for expansion?
Of course, the mere fact that governments and professional organizations have an interest in keeping consumer audio products and hearing aids safe for purchasers introduces boundaries and realms of influences. These can and have, on occasion, troubled the waters with rule changes that reshape the market dynamics. Any modeling of the economics should take into consideration influencers and boundary-setting agents as represented in Figure 5.
How Can PSAPs Be Dispenser-Friendly in a Sea of Threatening Changes?
There are several ways that PSAPs can be used beneficially in association with professional dispensing offices. First, advertising “Low Cost options to hearing aids” is one way if affordability is a significant component of the non-adopter purchasing calculus. This at first may seem starkly at odds with the natural proclivity for hearing professionals to sell and fit high-end hearing aid options. “Bundling” hearing aid costs with the extensive counseling and adjustment services is a fairly common practice in dispensing practices3. However, bundling may not always be the best strategy, especially when one is trying to attract new consumers in the “situational auditory stress” category.
It is also fundamental to every business to continuously seek new clients and to enlarge the population pool within the market. Clearly, many who may respond to a “low-cost” option hook may, in fact, be candidates for hearing aids, which offers an obvious opportunity for the adept dispenser with reasonable trade skill. Unquestionably, clearly separating the nature of PSAPs versus hearing aids is necessary. The PSAP is a consumer audio, off-the-shelf, product–period. There is no customization, no attribution of hearing loss treatment. Extensive audiometric testing is not a part of the transaction. In contrast with the considerable time and expertise applied to hearing aid evaluation, fitting, and validation, the contact can be as simple as, “Here’s your PSAP. Good luck; thank you for coming in and giving me your name and details for future marketing. Don’t forget where we are located when you need more serious professional help, and be sure to tell your friends and family about us.” A new client is entered into the marketing file, and a small profit is made.
Clearly, that is a gross simplification, but it may contain the seeds of practicality. In some cases, there will be obvious and natural opportunities to engage the PSAP shopper with the suggestion of a complimentary “hearing check” (as distinct from a comprehensive audiometric examination). This may or may not lead to an enhanced opportunity to discuss the virtues of custom-programmed and skillfully delivered hearing aids, as opposed to the PSAP option. Additionally, the engagement with new consumers will provide them with a definitive understanding of where to find competent professional services when needed for themselves or for others.
Does this type of marketing damage the reputation of the dispenser with their existing client base who may ask why their products cost so much more? Clearly, that risk can be averted with appropriate message controls that explicitly explain that the low-cost consumer options are not hearing aids, which are carefully selected and fit hearing loss treatment products. It is also worth noting that some business analytics suggest that the average marketing cost for a practice to acquire a new hearing aid client is as high as $500. On this basis, the trade-off of overcoming the inertial resistance associated with expanding into the new PSAP market may be well worth considering.
With regard to the “hearing check” component, many professionals, audiologists especially, have wrestled with devaluing the diagnostic component of their expertise by offering “free” testing. But most consumers can be reasonably assumed to appreciate the difference between a comprehensive audiologic evaluation, including the identification of medically significant symptoms, versus a gross profile of auditory performance. Kiosks have long populated grocery and pharmacy stores for blood pressure without the presumption that a full cardiovascular work up has been obtained. Online hearing checks have appeared over the past decades in various forms, as have “hearing check” kiosks (the author had several pre-digital kiosks located in shopping malls 20 years ago).
New digital versions may be strategically located either within a dispensing office to allow a curious, but not committed, consumer to explore his hearing on a gross basis, or in a remote location, such as a local pharmacy or senior center. In the latter case, the kiosk can be used to promote and identify the associated hearing professional’s office in high traffic remote locations. Interested consumers can instantly request their report to be emailed and the interaction is relayed to the host practitioner.
In the case of the Able Planet version of the Free Hearing Check Kiosk, it can additionally serve to allow the consumer to purchase consumer audio products online with a portion of the profit (and the market details) routed to the sponsoring practice’s office. This approach has the immediate effect of reaching out to the large pool of medically averse consumers who willfully avoid going into hearing aid offices until some tipping point of difficulty with their hearing reaches a full time level of urgency. It should be noted that the hearing check kiosks are just a small part of the expanding technology-enabled growth of telemedicine.
Finally, it can be argued that the boundaries suggested in Figure 1 between the pool of hearing aid candidates (long considered inadequately reached by suppliers) and the much larger one of PSAP consumers is a porous and dynamic division at best. In the tidy, discrete world of presumed (or preferred) distinctions, the separation is unambiguous, as suggested in Figure 6.
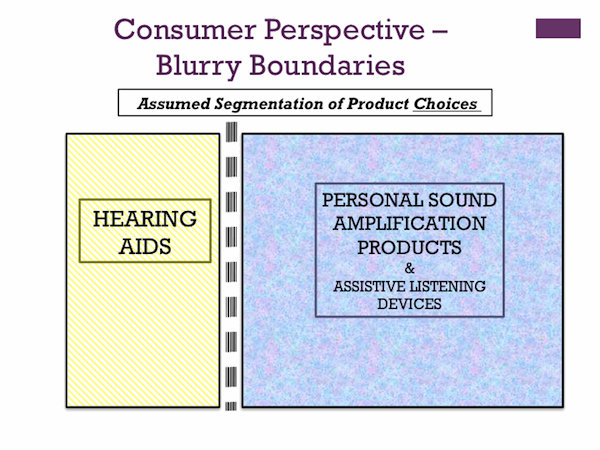
Figure 6. Product choice segmentation by traditional assumptions showing a clear separation of Hearing Aids (Medical Devices) and Assistive Listening devices, including Personal Sound Amplification Products.
The boundaries drawn in Figure 6 are largely a matter of regulatory map making. To be sure, no sensible manufacturer would attempt to bypass the guidelines issued by the FDA, and, as previously noted, there are many important differences in delivery of hearing aids with their attendant professional services from that of personal sound amplification products. Likewise, there is nothing to suggest that the service-intensive, high dollar hearing aid practice will vanish. A market for high-end hearing aids with professional stewardship will no doubt persist, even if as a relatively small niche.
But, in fact, PSAPs are simply small versions of Assistive Listening devices that happen to look and behave in ways very similar to hearing aids. To a reflective consumer the well-programmed hearing aid is a personal amplifier! Should there be rules (from FDA? FTC?) to limit how good PSAPS should be? No noise reduction allowed? No feedback cancellation, or multi-channel compression permitted? That is clearly a preposterous notion, completely anathema to the spirit and premise of progress and free market economics, one that consumers would rightly protest. Hence, the stark boundary of Figure 6 will likely have much greater porosity and ambiguity at the edges as these changes proceed in the coming years.
This is the assertion of Figure 7, a speculation postulated in the full recognition of the importance of professional audiological and otological care and the danger of untreated ear and hearing disease. But at the same time, as Mark Ross4, a long-time icon of audiology and hearing aid consumer advocate, has indicated – some hearing help is better than no hearing help. There is a continuing need for professional intervention, but not to the exclusion of a little help for many. This is particularly important in light of, and made much more urgent by, the expanding evidence of the impact on brain function in late life when even mild hearing difficulties persist without amplification.5,6
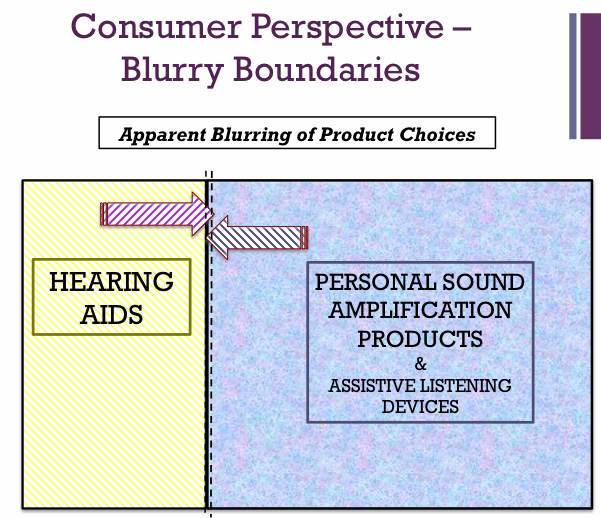
Figure 7. Illustration of the emerging Blurriness in product segmentation as PSAPs are increasingly purchased as Entry Level amplification, in some cases upgradeable, customized and then registered as Hearing Aids.
Medicare and Medicaid and private medical insurance have been facing highly publicized pressures for significant change in recent years, the Affordable Health Care Act of 2010 being the most recognizable example. Clearly, these politically contentious and momentous changes are unsettled and evolving. But cost containment is most certainly high on the priority list among the discussions of how it will sort out. Meanwhile, the huge increase in retirement age “Active Baby Boomers” (or Zoomers, older folks who “zoom about with a zest for living”) who may need some amount of hearing help, on a part-time, non-medical basis, makes it hard not to presume that the market for PSAPs is at the beginnings of a significant enlargement. Furthermore, the decidedly lower-priced PSAPs may also serve a role in auditory assistance for low-income persons, as well as individuals in highly circumscribed environments, such as nursing homes or assisted living facilities where non-professionally fit, lower cost options may be attractive solutions.
(Next Week: Trimming the Sails – Part IV)
References and Footnotes
1Oligopoly. AmosWEB Encyclonomic WEB*pedia
2HIA: Hearing Aid Sales Up 2.9% in 2012. Hearing Review Interactive Edition.
3Ross, M. (2012) Direct to Consumer Services – Comment on the hi Hearing Innovations Hearing Aid Dispensing Program. Hearing Loss Magazine March/April 28-30.
4Ross, M. (2012) Direct to Consumer Services – Comment on the hi Hearing Innovations Hearing Aid Dispensing Program. Hearing Loss Magazine March/April 28-30.
5Lin FR, Metter EJ, O’Brien RJ, Resnick SM, Zonderman A, Ferrucci L. (2011) Hearing loss and incident dementia. Arch Neurol. Feb;68(2):214-20.
6Beck DL and Edwards B, Humes LE, Lemke U, Lunner T, Lin FR, Pichora-Fuller MK. (2012) Expert Roundtable: Issues in Audition, Cognition, and Amplification Hearing Review,19(09):16-26.









What a nicely timed piece. Way to go, Chris. All this time, I thought that “oligopoly” was that company that made gym bags. On a serious note, wouldn’t it be interesting to tell us which companies are owned or controlled in various manners by the big 6? Many people in the field don’t know who belongs to whom. Looking forward to Part IV.