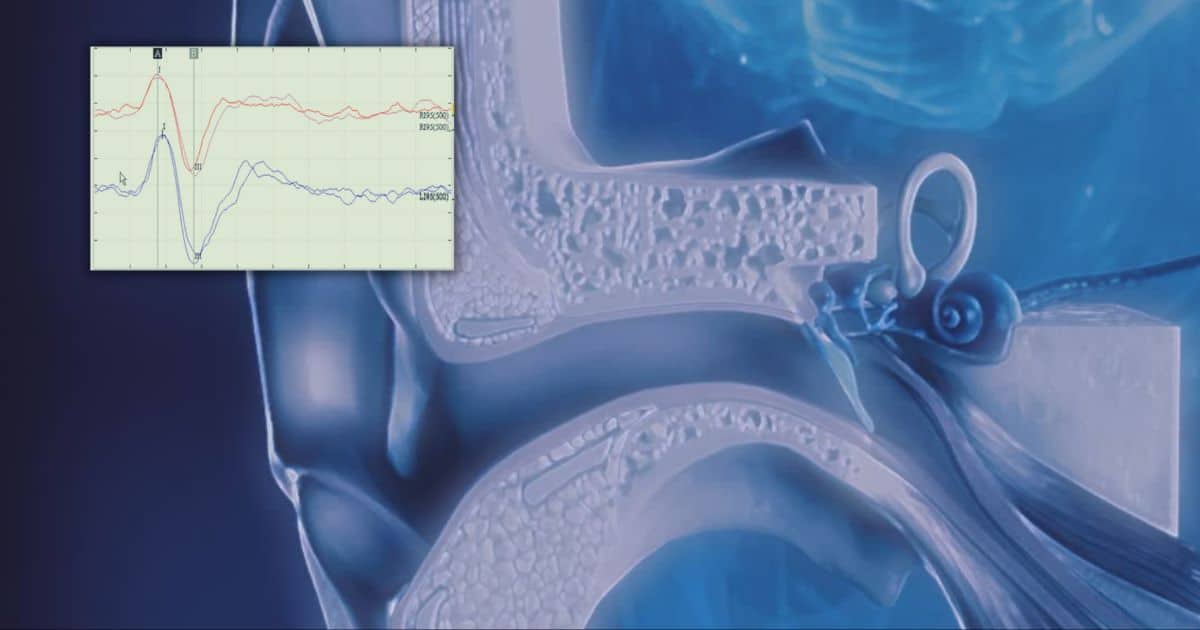
Editor’s Note: Brady Workman is back this week with a follow up to a post from several months ago VEMPs: what are they good for? This week’s post will instead focus on what the scientific evidence shows VEMPs are good for.
The vestibular evoked myogenic potential (VEMP) is a relatively new means of vestibular assessment, which only received FDA approval in 2015. As such, the diagnostic utility and scientific evidence supporting the use of VEMP testing is still being investigated. The two primary VEMP responses investigated in the literature are the cervical VEMP, also known as a cVEMP, and the ocular VEMP, or oVEMP. These responses are believed to be measures of otolith function (linear sensors of the inner ear), with the cVEMP thought to assess saccular function and the inferior branch of the vestibular nerve and the oVEMP thought to assess utricular function and the superior branch of the vestibular nerve.
Readers unfamiliar with these two VEMP responses are referred to one of my previous posts Vestibular Evoked Myogenic Potential (VEMP) for the basic characteristics of these measures.
Recently the American Academy of Neurology released a clinical practice guideline for the use of cVEMPS and oVEMPS with a systematic review of the available evidence. The primary objectives of this were to determine if VEMPs identify superior canal dehiscence syndrome (an abnormal thinning of bone in the superior semicircular canal), if VEMPs identify otolith dysfunction, and if VEMPs aid in diagnosis of other specific vestibular disorders.
Do VEMPs aid in the diagnosis of superior canal dehiscence syndrome (SCDS)?
The use of cVEMP threshold values was found to be 86-91% sensitive and 90-96% specific in separating individuals with SCDS confirmed by imaging from controls. The use of cVEMP amplitude measures, when appropriately corrected for electromyographic (EMG)/ muscle activity, was found to be 100% sensitive and 93% specific in separating those with SCDS confirmed by imaging from those without.
The use of oVEMP threshold value was found to potentially distinguish SCDS from control subjects with 77% sensitivity and 93% specificity when thresholds were found to be significantly below clinic normative data (2 standard deviations). The use of oVEMP amplitude value was found to be 77-100% sensitive and 98-100% specific at separating control subjects from those with SCDS.
Those with SCDS tend to have lower thresholds for VEMP measures due to the abnormal thinning of bone in the superior semicircular canal. This thinning of bone alters the fluid dynamics of the fluid filled vestibular system and allows for the measurement of VEMP responses at lower sound levels and with larger amplitudes than in patients without SCDS.
Do VEMPs identify otolith specific dysfunction?
The current evidence available did not allow the authors to determine if VEMPs specifically identified saccule and/or utricle dysfunction because no current reference standard for isolated otolith dysfunction exists. There is a general consensus, however, that the cVEMP is closely connected with saccule function and the oVEMP with utricle function.
Do VEMPs aid in diagnosis of other vestibular disorders?
Vestibular Neuritis (inflammation of vestibular nerve)
Expert consensus supports using cVEMP and/or oVEMP to determine the extent to which vestibular neuritis has affected the vestibular system. Current evidence suggests that VEMPS cannot specifically identify affected vestibular structures alone. For example, an abnormal cVEMP on the side of caloric hypofunction would imply involvement of both the superior and inferior branches of the vestibular nerve.
Meniere’s Disease (fluid abnormality of the ear)
VEMPs alone are not useful in making the diagnosis of Meniere’s disease, but may be used as accessory test to quantify peripheral vestibular damage as a result of Meniere disease.
Benign Paroxysmal Positional Vertigo (BPPV) (migrated ear particles)
VEMPs are not currently useful in making a diagnosis of BPPV type vertigo.
Vestibular Migraine
Some patients with vestibular migraine have been shown to have absent or reduced amplitude VEMPs in either one or both ears; however, currently VEMPs cannot be used to aid in the diagnosis of vestibular migraine.
So, what does the evidence show?
Currently, VEMPs are useful in making a diagnosis of superior canal dehiscence syndrome and as an ancillary test to quantify the extent of vestibular system damage in relation to other primary vestibular disorders.
More research is necessary to further determine the roles of VEMP measures in the clinical evaluation of patients with otologic and/or neurologic conditions. Standardization of test protocols is necessary to further prove VEMPs as effective clinical tools and to allow for more widespread clinical use.